
While running is the go-to aerobic exercise of choice for many individuals, according to recent studies, anywhere from
1-in-5 to 1-in-2 runners experience a running-related injury when observed over a one year period of time.
While marathoner runners appear to be at the highest overall risk when it comes to the likelihood of incurring a running-related injury, casual or novice runners are not immune to the odd, nagging injury.
Though it’s impossible to predict the future, steps can be taken by both novice and seasoned runners to both prevent common running injuries and address an injury should it occur.
What are the top three most common running injuries?
Pound for pound, the three most common running injuries are patellar tendinopathies, patellofemoral pain syndrome, and hamstring strains (“tears”).
Patellar tendinopathies:
Patellar tendinopathies, which includes patellar tendinitis, is the most common group of knee injuries suffered by runners. Often characterized by sharp, pinpointed pain in the knee, these injuries are also associated with jumping, landing, and running activities. They are largely considered overuse injuries thought to be caused by excessive repetitive force through the patellar tendon.
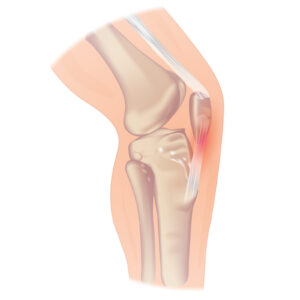
Patellofemoral Pain Syndrome (PFS):
Patellofemoral Pain Syndrome is a common running injury that can plague runners in one or both knees simultaneously, and has the unfortunate reputation of reappearing after apparent resolution. Most people suffering from PFS experience vague knee pain around or under the patella (“knee cap”). Symptoms tend to be at their worst when weight bearing with a flexed knee during activities such as squatting, going up and down stairs, running, and with hopping or jumping activities.
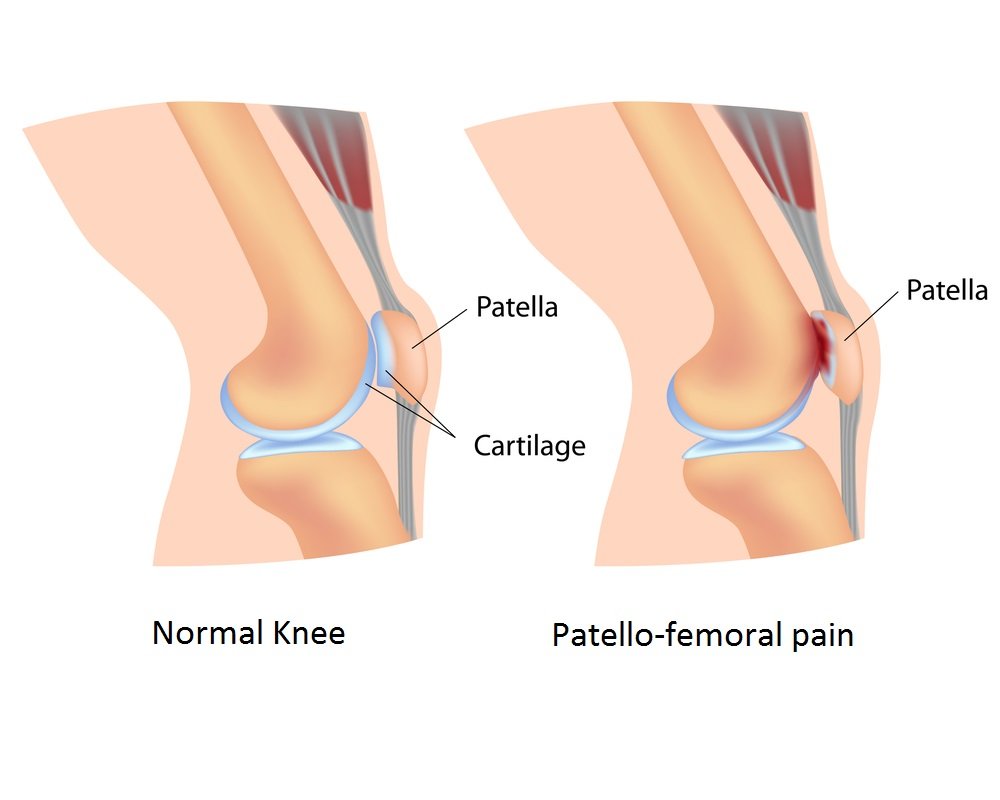
Hamstring strains: Hamstring injuries are among the most common, non-contact injuries in sports accounting for over 12% of all lower extremity sport injuries. These injuries can require extensive treatment and long rehabilitation periods depending on the severity of the injury and where the injury occurs. Also, previous hamstring injury has been found by multiple studies to be the greatest risk factor for development of a future hamstring injury with a recurrence rate of 12-33% even with preventative measures.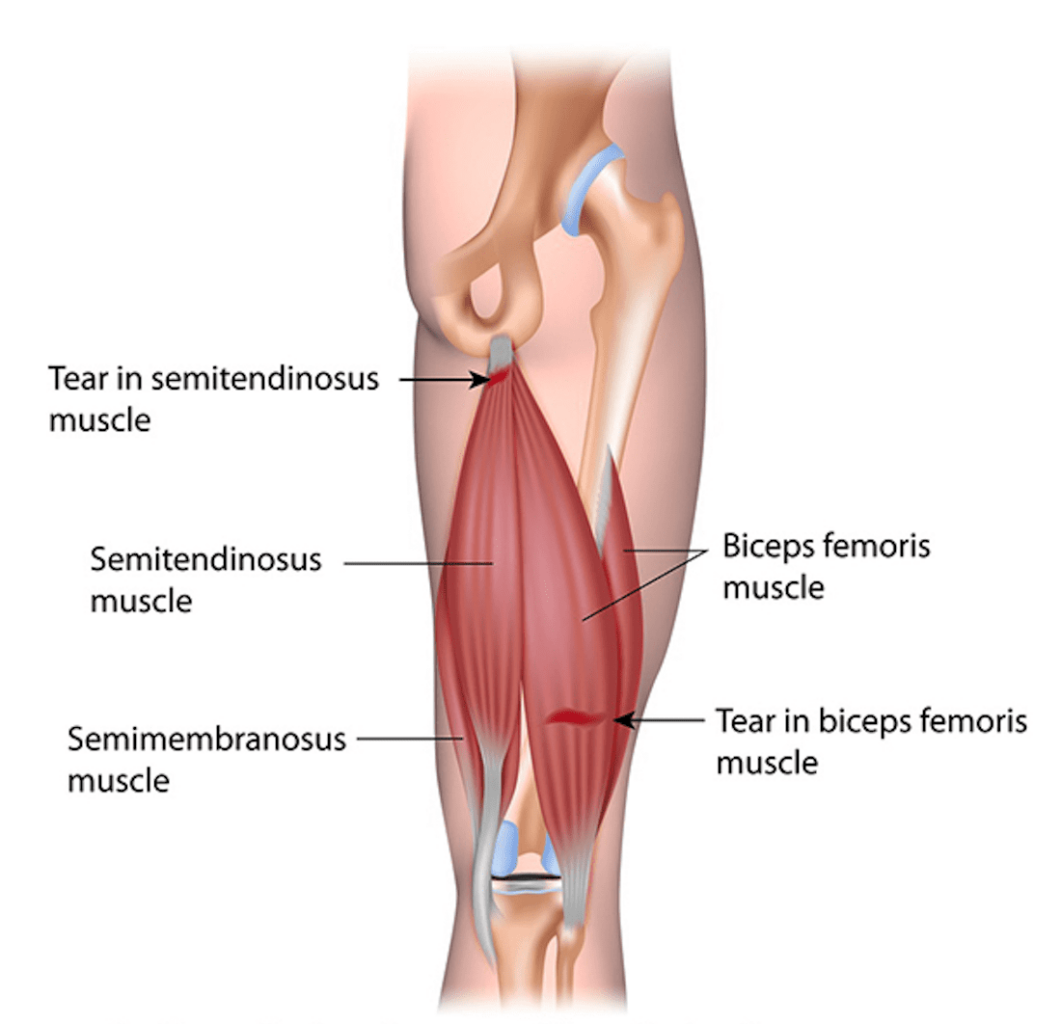
What causes these common running injuries?
A whopping 80% of all common running injuries can be attributed to overuse.
Overuse, in this context, is defined as repetitive or chronic trauma to a tissue ultimately resulting in injury. In other words, it wasn’t just the first or maybe even the fifth time your activity put too much stress or strain on a given tissue, but chronic “use-and-abuse” ultimately culminates in pain and dysfunction that your body will no longer allow you to ignore. High velocity activities can also vie for a place at the top of the injury list.
In the case of hamstring strains (“tears”), high impact activities like sprinting are often associated with an acute rupture of these tissues. Pinpointing one factor that stands out among those contributing to injury can certainly prove elusive. However, there are common areas that, when addressed, can reliably lead to injury prevention including warm-ups and improving muscle imbalances, muscular endurance, and muscular flexibility.
Furthermore, research shows that, left unaddressed, muscle imbalances, muscle fatigue, muscle “tightness”, insufficient warm-up, and prior injuries have an additive effect, such that “exceeding a threshold of cumulative risk factors has been hypothesised to result in an injury.”
Unfortunately, there isn’t one quick fix to resolve all potential factors that may result in an injury. The good news is that addressing the modifiable factors mentioned above can give runners a “leg up” when it comes to reducing injury risk factors.
Can these common running injuries be prevented?
Patellar Tendinopathy
While there is limited evidence and research surrounding specific prevention strategies for patellar tendinopathy, there are commonalities that exist among those who end up experiencing symptoms. They include:
- Decreased quad and hamstring flexibility
- Abnormal patellar tracking
- High training volume
- Training on concrete surfaces
- Sports specialization
If you end up with a patellar tendinopathy diagnosis, recent research suggests targeted approaches to addressing your symptoms. Below are a few different approaches to addressing patellar tendinopathy that have good support from recent research. Also, to help guide your treatment plan, talk with your healthcare providers to help you select and follow through with a treatment strategy.
Long term strategies supported by a 2019 systematic review focusing on treatment of patellar tendinopathies include: Eccentric exercises such as decline squats, dry needling (DN) with platelet-rich plasma (PRP), autologous blood injection (ABI) and saline injections. These strategies have been shown to provide both functional improvements as well as long-term pain relief. Additionally, heavy slow resistance (HSR) protocols including squats, leg press, and hack squats show both short and long term effects on tendons at a cellular level.
For short term, same-day, temporary decreases in pain, isometric exercises, patellar strapping, and targeted taping techniques have shown good results. However, none of these strategies provided long-term solutions to addressing patellar tendinopathy.
Patellofemoral Syndrome (PFS) or Patellofemoral Pain Syndrome (PFPS)
Unfortunately, the most current evidence doesn’t support any significant findings when it comes to specific recommendations to avoid developing PFS. However, research has shown there are common factors that make a person more likely to develop PFS, including:
- Overuse and overtraining that exceeds the ability of the tissue to recover between exercise training sessions
- Movement and coordination deficits
- Muscle performance deficits
- Decreased mobility through the patellar retinaculum
- Excessive foot pronation
An early, strengthening treatment program for hips, knees and feet as well as pelvic stabilization may help pain from PFS from becoming chronic.
Additionally, high-level evidence from 4 randomized controlled clinical trials found that exercises that help strengthen hip muscles including abductors, external rotators, and extensors improve symptoms associated with PFS.
Furthermore, making sure to add exercises focused on strengthening and stretching the hamstrings, calf muscles, and quadriceps as well as improving iliotibial band (IT band) mobility also contributed to improved symptoms when combined with hip strengthening activities. An example of exercises used in these particular studies by the subjects included:
– Strengthening exercises targeting the hip abductors, external rotators, and extensors, including 2-4 sets of 10-15 repetitions each.
– Stretching exercises held for 30 seconds and performed 3 times consecutively at a minimum of 3 times per week for 4 weeks.
Hamstring Injuries
When dealing with a hamstring tear, or if you’re trying to improve the odds of preventing one, high quality, well supported clinical trials support specific hamstring strengthening exercises that can be used for both injury prevention and recovery. These studies have identified specific commonalities that likely increase the risk of developing a hamstring injury, including muscle fatigue and impaired neuromuscular control.
Fatigue is consistently associated with hamstring injury and has been demonstrated to impair neuromuscular function. Additionally, hamstring re-injuries are found more commonly in athletes with strength-endurance deficits. In these athletes, the injured muscle fatigues “earlier and demonstrates altered activation patterns as well as a higher incidence of injuries occurring during the final third of training sessions.”
Keeping these factors in mind, it should come as no surprise that exercises targeting improved endurance and neuromuscular function show good results in injury prevention as well as recovery after an injury has occurred. Additionally, strength training of the hamstrings under fatigue has demonstrated positive effects on hamstring function and reduced injury rates.
Here are some examples of exercises shown to both prevent and address hamstring injuries:
– A systematic review and meta-analysis published by Al Attar W et al in 2017 found strong evidence that training programs that include Nordic Hamstring (NH) exercises decrease the risk of hamstring injuries by up to 51 % in the long term compared with usual warm-up or training programs.

– A study published in 2020 states that “Neural adaptations also occur following Nordic Hamstring (NH) programs, with higher hamstring muscle activation during the NH exercise after a 6-week intervention.” The study goes further to conclude that improvements in muscle activation combined with no change in quadriceps muscle activation suggested that NH training improves neuromuscular control.
– In addition to Nordic Hamstring exercises, the single-leg Roman Chair hold, with longer duration muscle contractions, was found to be more effective at increasing hamstring muscle endurance than Nordic Hamstring exercises. This suggests that isometric training may be a useful addition to eccentric loading to condition the hamstrings when the goal is to improve fatigue resistance.
What to do if you’ve already started to feel symptoms
If you find yourself dealing with persistent symptoms that are unresponsive to rest and modification of your training schedule or technique, seeking out the advice of a healthcare professional who is qualified to assess your symptoms can help you rule out more serious issues, and recommend an appropriate course of treatment.
Healthcare providers, including Physical Therapists can help you establish a safe and effective approach to addressing your symptoms or injury.
References
1. Al Attar W, Soomro N, Sinclair P, Pappas E, Sanders R. Effect of Injury Prevention Programs that Include the Nordic Hamstring Exercise on Hamstring Injury Rates in Soccer Players: A Systematic Review and Meta-Analysis. Sports Medicine.2017;47(5):907.
http://search.ebscohost.com/login.aspx?direct=true&db=edb&AN=122540540&site=eds-live.
Accessed May 14, 2020.
2. k SV, Bueno AM, Nielsen RO, Rasmussen S. Incidence of running-related injuries per 1000 h of running in different types of runners: A systematic review and meta-analysis. Sports Medicine. 2015;45(7):1017-1026. https://search.proquest.com/docview/1716904639?accountid=41004.
3. Ramskov D, Barton C, Nielsen RO, Rasmussen S. High Eccentric Hip Abduction Strength Reduces the Risk of Developing Patellofemoral Pain Among Novice Runners Initiating a Self-Structured Running Program: A 1-Year Observational Study. Journal of Orthopaedic & Sports Physical Therapy. 2015;45(3):153-161. doi:10.2519/jospt.2015.5091.
4. Reinking MF. Current Concepts in the Treatment of Patellar Tendinopathy. International journal of sports physical therapy. 2016;11(6):854-866. http://search.ebscohost.com/login.aspx?direct=true&db=cmedm&AN=27904789&site=eds-live
5. Seymore K, Domire Z, DeVita P, et al. The effect of Nordic hamstring strength training on muscle architecture, stiffness, and strength. European Journal of Applied Physiology. 2017;117(5):943.
http://search.ebscohost.com/login.aspx?direct=true&db=edb&AN=122421282&site=eds-live.
Accessed May 31, 2020
6. Trevor VD, Jelley W. Non-surgical treatment of patellar tendinopathy: A systematic review of randomized controlled trials. Journal of Science and Medicine in Sport. 2020;23(2):118-124. https://search.proquest.com/docview/2334166666?accountid=41004. doi:http://dx.doi.org/10.1016/j.jsams.2019.09.008.
7. van der Horst N, Smits DW, Petersen J, Goedhart EA, Backx FJ. The preventive effect of the nordic hamstring exercise on hamstring injuries in amateur soccer players: a randomized controlled trial. Am J Sports Med. 2015;43(6):1316‐1323. doi:10.1177/0363546515574057
Holly Brownstein, DPT

This post was written by Dr. Holly Brownstein in August of 2021.
Learn more about Andrew on our about page: https://gopt.co/about/